Health System Financing
|
Policy makers face multiple decisions regarding how a health system collects the necessary funding, how it pools these funds so all members bear the financial risks of illness and ease the financial barriers to access necessary services (the health insurance function in health financing), and how it uses them to pay for population and individual health services. All these decisions have very significant equity and financial implications for societies, governments and households as well as for labor markets and country global competitiveness. Health financing arrangements play a large role in determining access to necessary health services, in protecting members from the impoverishing effects of illness, and to large extent, in providing incentives to improve quality, health prevention, responsiveness, and productivity for health service providers. In many cases it also has substantial implications for a country's fiscal performance.
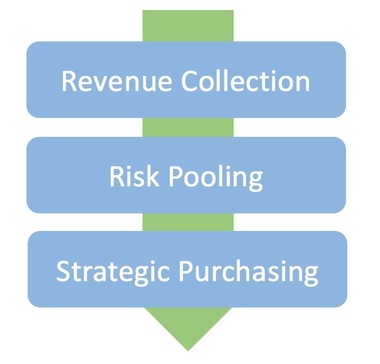
In CHD we work with, provide advice, and train as needed, our partners and global and country leaders on design options and implementation strategies on critical health system financing areas: Revenue Collection, Risk Pooling and Strategic Purchasing. |
Revenue CollectionHow to Fund
the Health System ? Policy makers and systems leaders face a multiplicity of options to fund the system from general government revenues to taxes to the payroll, insurance premiums, sin taxes and fees. Decisions on sources and levels of funding have substantial impact on fiscal sustainability, global country competitiveness, labor markets, access to services, financial protection, and equity. All of them need to be examined when making decisions of sources, levels and mechanisms for revenue collection.
CHD supports countries and public and private system leaders in identifying best options, assessing the impacts, and defining implementation and transition strategies to fund the system. |
Risk Pooling
How to Organize and
Optimize Health Insurance ? How collected funds are managed, specifically how they are aggregated to provide coverage for participants is essential to determine the capacity of the health system to increase access to necessary services and to reduce the financial risk when facing illness and accidents. The aggregation of funds in a pool is known as risk pooling (or the health insurance function in a health system). Affective risk pools allow for all participants rather than one individual to share the financial risk of illness.
Policy makers and system leaders face options and challenges when organizing risk pooling (insurance). Should they choose single insurer or multiple?; social insurance or private insurance?; competing or not competing?; self regulation or public regulation?; and many others. CHD has substantial and distinctive experience and expertise in supporting countries and leaders in identifying options, assessing their feasibility and implications and develop the implementation and transition strategies. |
Strategic PurchasingHow to Fund Provision
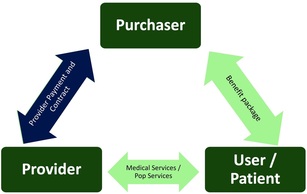
and Service Providers ? Once pooled, the use of funds for ensuring access to public health and personal health care services is the final step in the health financing cascade. It defines the incentive framework for providers and professionals contributing to health for quality, responsiveness, cost/effectiveness, and productivity. It also defines the funding flows for provider operations and sustainability.
Use of funds has at least four key challenges for any health system:
|